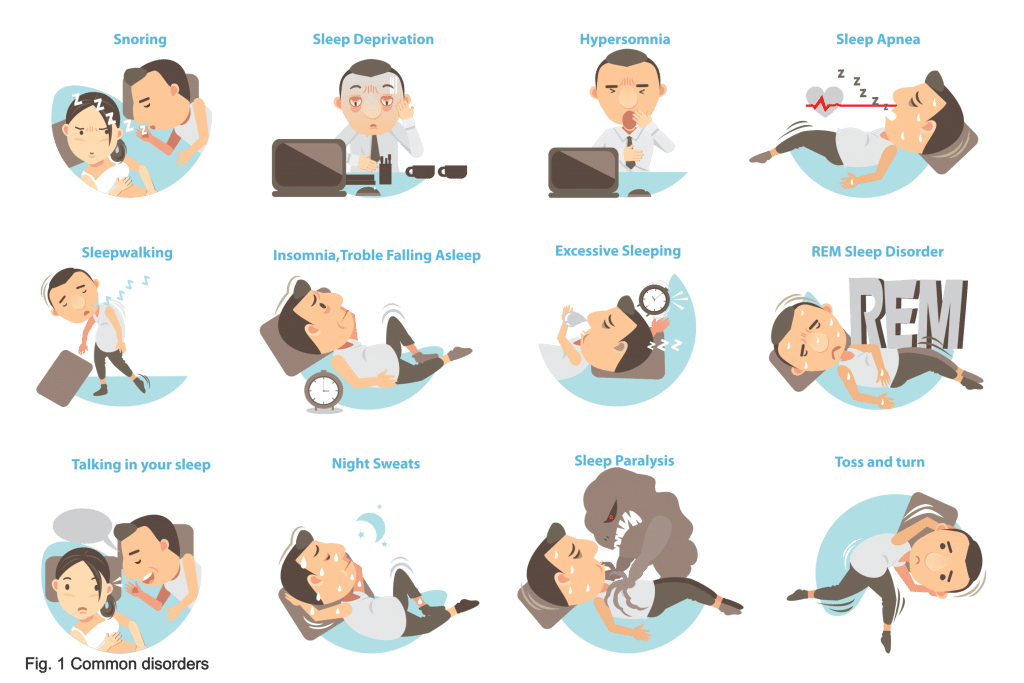
Sleep disorders are a prevalent issue that affects many individuals worldwide. This article aims to illuminate some of the most common sleep disorders, unveiling their symptoms, causes, and potential treatments.
Have you ever wondered why you struggle with falling asleep or waking up frequently at night?
Join us as we explore the fascinating world of sleep disorders and gain a deeper understanding of these disruptive conditions that can hinder our restful nights and affect our overall well-being.
Review contents
Insomnia
Insomnia is a sleep disorder that affects a significant number of people worldwide. It is characterized by difficulty falling asleep, staying asleep, or both. As a result, individuals with insomnia often experience chronic fatigue, lack of concentration, irritability, and impaired daily functioning.
Insomnia symptoms vary from person to person. Still, common signs include difficulty falling asleep, waking up frequently during the night, waking up too early in the morning, and feeling unrefreshed after sleep.
The causes of insomnia are numerous and can be both physical and psychological. Some physical factors contributing to insomnia include underlying medical conditions like chronic pain, asthma, allergies, and gastrointestinal problems.
Hormonal changes, such as those experienced during pregnancy or menopause, can disrupt sleep patterns. Additionally, certain medications, caffeine, nicotine, and alcohol can interfere with sleep quality. Psychologically, stress, anxiety, depression, and traumatic experiences can play a significant role in the development of insomnia.
When it comes to treating insomnia, there are various options available. Non-pharmacological approaches include practicing good sleep hygiene, which involves maintaining a consistent sleep schedule, creating a relaxing bedtime routine, and ensuring a comfortable sleep environment.
Cognitive-behavioral therapy for insomnia (CBTI) is also an effective treatment that helps individuals identify and change the thoughts and behaviors contributing to sleep problems. Medication may sometimes be prescribed to help regulate sleep patterns, but its long-term use should be carefully monitored and evaluated.
Sleep Apnea
Sleep apnea is a severe sleep disorder characterized by interruptions in breathing during sleep. These pauses in breathing can occur multiple times throughout the night and last for seconds to minutes. Sleep apnea is classified into three types: obstructive sleep apnea, central sleep apnea, and complex sleep apnea syndrome.
The most common sleep apnea symptoms include loud snoring, gasping or choking sounds during sleep, restless sleep, daytime sleepiness, morning headaches, and difficulty concentrating. Obstructive sleep apnea, the most prevalent form, occurs when the muscles in the throat relax and block the airway. Central sleep apnea is caused by a failure of the brain to send appropriate signals to the muscles that control breathing. Complex sleep apnea syndrome is a combination of both obstructive and central sleep apnea.
The causes of sleep apnea can vary depending on the type. Obstructive sleep apnea is often associated with obesity, as excess weight can pressure the airway. However, it can also be caused by structural abnormalities in the throat, such as enlarged tonsils or a deviated septum.
Central sleep apnea can result from certain medical conditions like congestive heart failure, stroke, or brainstem injury. Additionally, lifestyle factors such as alcohol and sedative use can worsen sleep apnea symptoms.
Treatment options for sleep apnea depend on the severity and type of the disorder. Lifestyle changes are often recommended, such as losing weight, quitting smoking, and avoiding alcohol and sedatives. Continuous positive airway pressure (CPAP) therapy is a standard treatment method that involves wearing a mask over the nose or mouth during sleep, which delivers a steady stream of air to keep the airway open.
In some cases, surgery may be necessary to correct structural abnormalities in the throat or remove excess tissue blocking the airway.
This image is the property of www.sleephealthfoundation.org.au.
Restless Leg Syndrome (RLS)
Restless Leg Syndrome (RLS) is a neurological disorder characterized by an irresistible urge to move the legs, often accompanied by uncomfortable sensations. These sensations are often described as crawling, tingling, itching, or pulling, and they typically worsen at night or during periods of rest. As a result, individuals with RLS often have difficulty falling asleep or staying asleep, leading to daytime fatigue and impaired mood and cognitive functioning.
The exact cause of RLS is not fully understood, but it is believed to be related to abnormalities in the neurotransmitters dopamine and iron in the brain. Certain factors can exacerbate or trigger RLS symptoms, such as pregnancy, iron deficiency, medications, and chronic diseases like kidney failure and diabetes. Genetics likely play a role as RLS tends to run in families.
Treatment options for RLS aim to alleviate symptoms and improve sleep quality. Lifestyle changes such as regular exercise, avoiding caffeine and alcohol, and establishing a relaxing bedtime routine can help reduce symptoms. For individuals with severe symptoms, medications that increase dopamine levels or regulate iron levels in the brain may be prescribed. Treating underlying medical conditions or addressing iron deficiencies can sometimes alleviate RLS symptoms.
Narcolepsy
Narcolepsy is a neurological disorder characterized by excessive daytime sleepiness, sudden loss of muscle tone (cataplexy), hallucinations, and sleep paralysis. These symptoms can significantly impact daily life, as individuals with narcolepsy often struggle to stay awake during regular waking hours and experience disruptions in sleep patterns.
The exact cause of narcolepsy is not fully understood, but it is believed to involve a combination of genetic and environmental factors. Research suggests that narcolepsy may be caused by a deficiency of hypocretin, a neurotransmitter that regulates wakefulness and sleep. In some cases, an autoimmune response may also contribute to destroying the cells that produce hypocretin.
Treatment options for narcolepsy focus on managing symptoms and improving daytime functioning. Stimulant medications, such as amphetamines and modafinil, are often prescribed to help individuals stay awake and alert during the day. Antidepressant medications can effectively treat cataplexy and reduce the frequency of hallucinations and sleep paralysis. In addition to medication, lifestyle modifications such as regular sleep schedules and planned naps can help individuals with narcolepsy manage their symptoms and improve sleep quality.
This image is the property of www.sleepandattentiondisorders.com.
Sleepwalking
Sleepwalking, also known as somnambulism, is a disorder characterized by complex behaviors performed during sleep. These behaviors can range from sitting up or walking to more complex actions like driving a car or preparing food. Sleepwalking episodes typically occur during the deepest stage of non-rapid eye movement (NREM) sleep and can last a few minutes to an hour.
The exact cause of sleepwalking is not fully understood, but it is believed to be related to genetic and environmental factors. Sleepwalking can run in families, suggesting a genetic predisposition. Additionally, certain factors can trigger or exacerbate sleepwalking episodes, such as sleep deprivation, fever, stress, and the use of certain medications or substances.
Prevention is vital when it comes to sleepwalking. Creating a safe sleep environment is essential, as it can help prevent injuries during sleepwalking episodes. This includes removing obstacles or hazards from the bedroom, such as sharp objects or clutter.
Maintaining a regular sleep schedule and ensuring adequate sleep can also help reduce the likelihood of sleepwalking. If sleepwalking poses a significant risk or disrupts daily functioning, medical intervention may be necessary. Consultation with a sleep specialist can help determine the best course of action and may include medication or behavioral therapies.
Nightmares
Nightmares are vivid and disturbing dreams that often wake individuals from sleep, leading to feelings of fear, anxiety, and distress. Nightmares can vary in intensity and content, but they typically involve threatening, dangerous, or emotionally distressing situations. Nightmares can be sporadic or frequent, significantly disrupting sleep and affecting overall well-being.
The exact cause of nightmares is not fully understood, but they are often associated with various emotional and psychological factors. Nightmare frequency and intensity can be influenced by stress, anxiety, trauma, certain medications, and psychological disorders such as post-traumatic stress disorder (PTSD). Nightmares are prevalent in young children and tend to decrease in frequency as individuals age.
Treatment options for nightmares typically focus on addressing underlying emotional or psychological factors. Therapy, such as cognitive-behavioral therapy for nightmares (CBT-N), can help individuals identify and modify the thoughts and feelings associated with nightmares.
Relaxation techniques, such as deep breathing exercises and progressive muscle relaxation, can also effectively reduce anxiety and promote better sleep. Medication may sometimes be prescribed to alleviate anxiety or other symptoms associated with nightmares, but its use should be carefully monitored.
This image is the property of ecosh.com.
Night Terrors
Night terrors, also known as sleep terrors, are intense episodes of fear and arousal that occur during sleep. Unlike nightmares, which occur during rapid eye movement (REM) sleep, night terrors happen during the first few hours of deep non-rapid eye movement (NREM) sleep.
During a night terror episode, individuals may scream, shout, or appear terrified, often accompanied by rapid breathing and an increased heart rate. They may also exhibit physical signs of distress, such as sweating or thrashing around.
The exact cause of night terrors is not fully understood, but they are believed to result from genetic and environmental factors. Night terrors can be triggered by stress, sleep deprivation, fever, sleep disorders, or certain medications. They are particularly common in children, with the prevalence decreasing as individuals reach adulthood.
Management of night terrors focuses on creating a safe sleep environment and ensuring the safety of the individual experiencing the episodes. During a night terror, it is important not to wake the individual forcefully, as this can cause confusion and distress.
Instead, gently redirecting them back to bed once the episode subsides is recommended. Addressing any underlying causes, such as sleep deprivation or stress, can also help reduce the frequency and intensity of night terrors. Medication or therapy may be prescribed to manage any associated anxiety or other sleep disorders in severe cases.
Hypersomnia
Hypersomnia is a sleep disorder characterized by excessive sleepiness and the desire to nap or sleep for extended periods. Unlike feeling tired from sleep deprivation, individuals with hypersomnia often struggle to stay awake and may experience difficulties functioning during waking hours.
Hypersomnia can significantly impact daily life and may be accompanied by symptoms such as difficulty waking up, sleep inertia (prolonged grogginess upon waking), and cognitive impairment.
The exact cause of hypersomnia is not fully understood, but it can be classified as either primary or secondary. Primary hypersomnia refers to cases where no underlying medical condition is causing the excessive sleepiness. Secondary hypersomnia, however, can result from other medical conditions such as sleep apnea, narcolepsy, or certain neurological disorders. Other factors like medication use, substance abuse, and certain genetic factors may also contribute to hypersomnia.
Treating hypersomnia involves identifying and addressing the underlying causes. For primary hypersomnia, lifestyle modifications such as maintaining regular sleep schedules, avoiding alcohol and sedatives, and practicing good sleep hygiene may help regulate sleep patterns.
In cases where hypersomnia is secondary to another medical condition, treating the underlying condition or adjusting medication may be necessary. Stimulant medications that promote wakefulness may also be prescribed to individuals with severe symptoms, but their use should be carefully monitored.
This image is the property of santacruzcore.com.
Bruxism
Bruxism is a sleep disorder characterized by the grinding or clenching of teeth during sleep. This condition can cause dental problems, jaw pain, headaches, and disrupted sleep for individuals with bruxism and their sleep partners. While occasional teeth grinding is common and usually harmless, chronic or severe bruxism can lead to dental damage, jaw disorders, and sleep disturbances.
The cause of bruxism is not fully understood, but it is believed to be multifactorial. Stress and anxiety are commonly associated with teeth grinding, suggesting that emotional factors play a role. Additionally, certain physical factors, such as misaligned teeth or an abnormal bite, can contribute to the development of bruxism. Sleep-related factors like sleep apnea and arousal may also be associated with bruxism.
Management of bruxism aims to protect the teeth, alleviate symptoms, and improve sleep quality. Wearing a custom-made mouthguard can provide a protective barrier between the upper and lower teeth, preventing further dental damage. Stress management and relaxation techniques like meditation or yoga can help reduce anxiety and muscle tension. Identifying and treating underlying sleep disorders, such as sleep apnea, can help alleviate bruxism symptoms.
Circadian Rhythm Disorders
Circadian rhythm disorders refer to disruptions in the natural sleep-wake cycle, leading to difficulties falling asleep, staying asleep, or being awake at the desired times. Several circadian rhythm disorders include delayed sleep-wake disorder, advanced sleep-wake disorder, irregular sleep-wake disorder, and shift work sleep disorder.
Symptoms of circadian rhythm disorders vary depending on the specific type but often include difficulty falling asleep or waking up at the desired times, excessive sleepiness during the day, and difficulty concentrating. Individuals with circadian rhythm disorders may experience chronic fatigue and impaired functioning due to the misalignment of their internal body clock with the external environment.
The causes of circadian rhythm disorders can be both genetic and environmental. Genetic factors can predispose individuals to specific sleep-wake patterns, making them more susceptible to circadian rhythm disruptions. Environmental factors, such as irregular work schedules, excessive light exposure at night, and irregular sleep patterns, can also contribute to the development of circadian rhythm disorders.
Treating circadian rhythm disorders involves regulating the sleep-wake cycle and establishing a consistent routine. Non-pharmacological approaches, such as light therapy, can help reset the internal body clock and promote better alignment with the desired sleep-wake times.
Good sleep hygiene practices, such as avoiding stimulants before bedtime and creating a sleep-friendly environment, can also aid in regulating sleep patterns. Medication may sometimes be prescribed to help regulate the sleep-wake cycle, but its use should be carefully monitored and evaluated.
This image is the property of www.tmjsleepcentre.net.au.